Microcurrent therapy is increasingly used in clinical and rehabilitation settings to support tissue repair, pain management, functional recovery, and post-surgical care. Its use is grounded in bioelectric principles that mirror the body’s natural signalling systems rather than overriding them. This overview highlights evidence-informed applications, observed benefits, and practical workflow considerations for healthcare professionals and well-informed patients. This content is educational only and not intended as medical advice. Treatment decisions should always be made in consultation with a licensed clinician.

Clinical & Medical Use Cases

Wound Care and Tissue Repair
Microcurrent therapy has been studied as an adjunctive tool for managing chronic and slow-healing wounds, including diabetic foot ulcers, venous leg ulcers, and pressure ulcers. Early clinical research demonstrated that low-level electrical stimulation can significantly accelerate wound healing rates compared to standard care alone (Cheng et al., Clinical Orthopedics and Related Research, 1982). In this study, enhanced ATP production was linked to faster cellular repair and tissue regeneration.
A review published in Advances in Wound Care reported that electrical stimulation therapies, including microcurrent modalities, were associated with improved wound closure rates and reduced healing time across multiple chronic wound types (Kloth, Advances in Wound Care, 2014). Another clinical observation noted improved tensile strength in healed tissue following microcurrent-supported wound care, suggesting stronger structural outcomes rather than superficial closure (Becker, The Body Electric, 1985).
Microcurrent therapy is not positioned as a standalone treatment. It is typically used alongside conventional wound management strategies such as dressings, pressure offloading, infection control, and medical supervision.
Pain Management as Adjunct Therapy
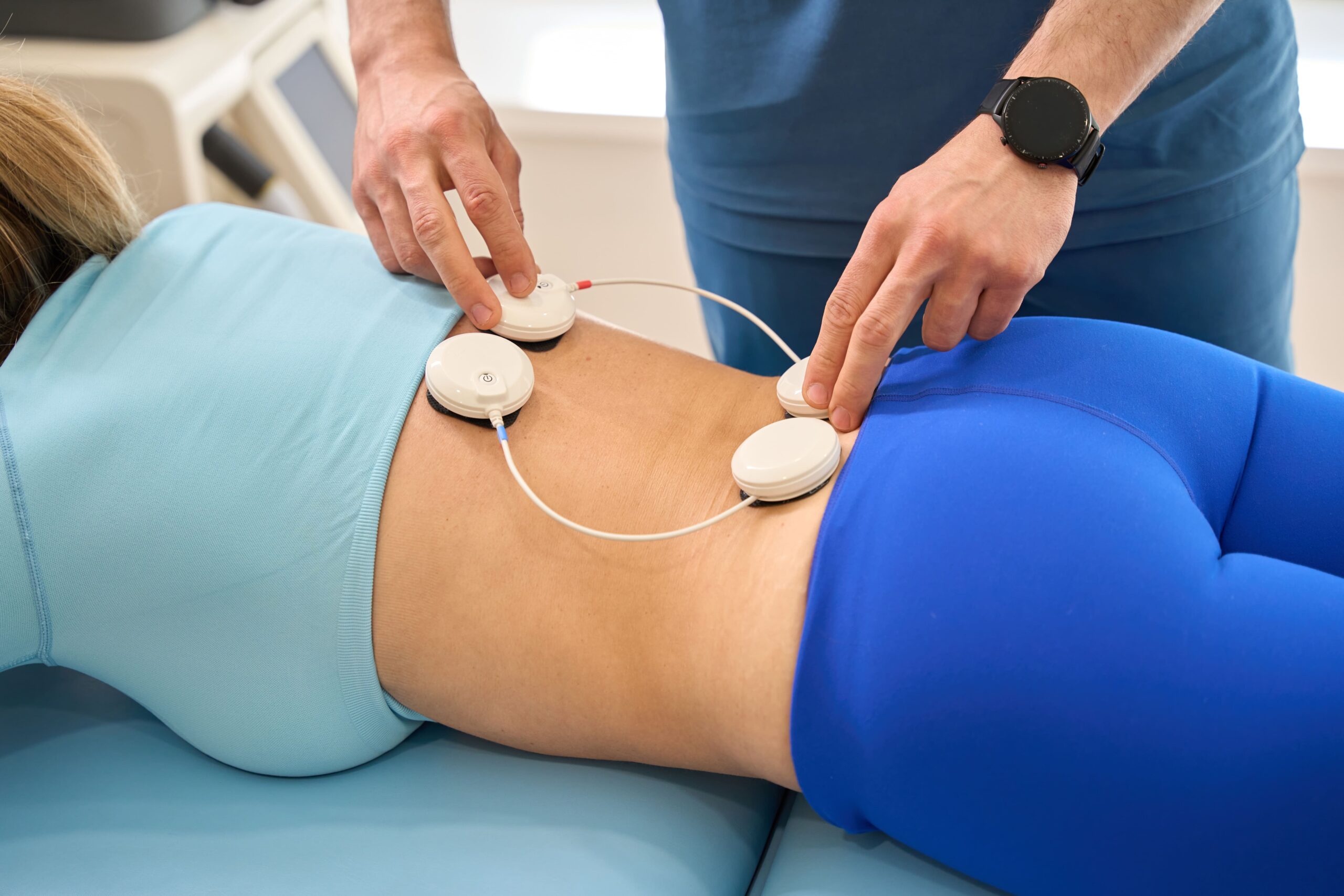
In musculoskeletal and post-operative settings, microcurrent therapy is used to complement existing pain management approaches rather than replace them. Unlike sensory-level stimulation, microcurrents operate below perception and aim to support physiological repair mechanisms that influence pain over time.
Clinical educator Carolyn McMakin reported that microcurrent therapy was associated with significant pain reduction in patients with chronic soft tissue injuries when used as part of a multimodal care plan (McMakin, Clinical Perspectives on Microcurrent Therapy, 2004). Another study found measurable reductions in pain scores without muscle contraction or sensory discomfort, supporting its role in sensitive or post-surgical populations (Lambert et al., Journal of Bodywork and Movement Therapies, 2002).
These findings reinforce that microcurrent therapy does not simply mask pain. Instead, it supports the biological conditions that allow pain to resolve more naturally as tissue function improves.

Rehabilitation and Sports Medicine
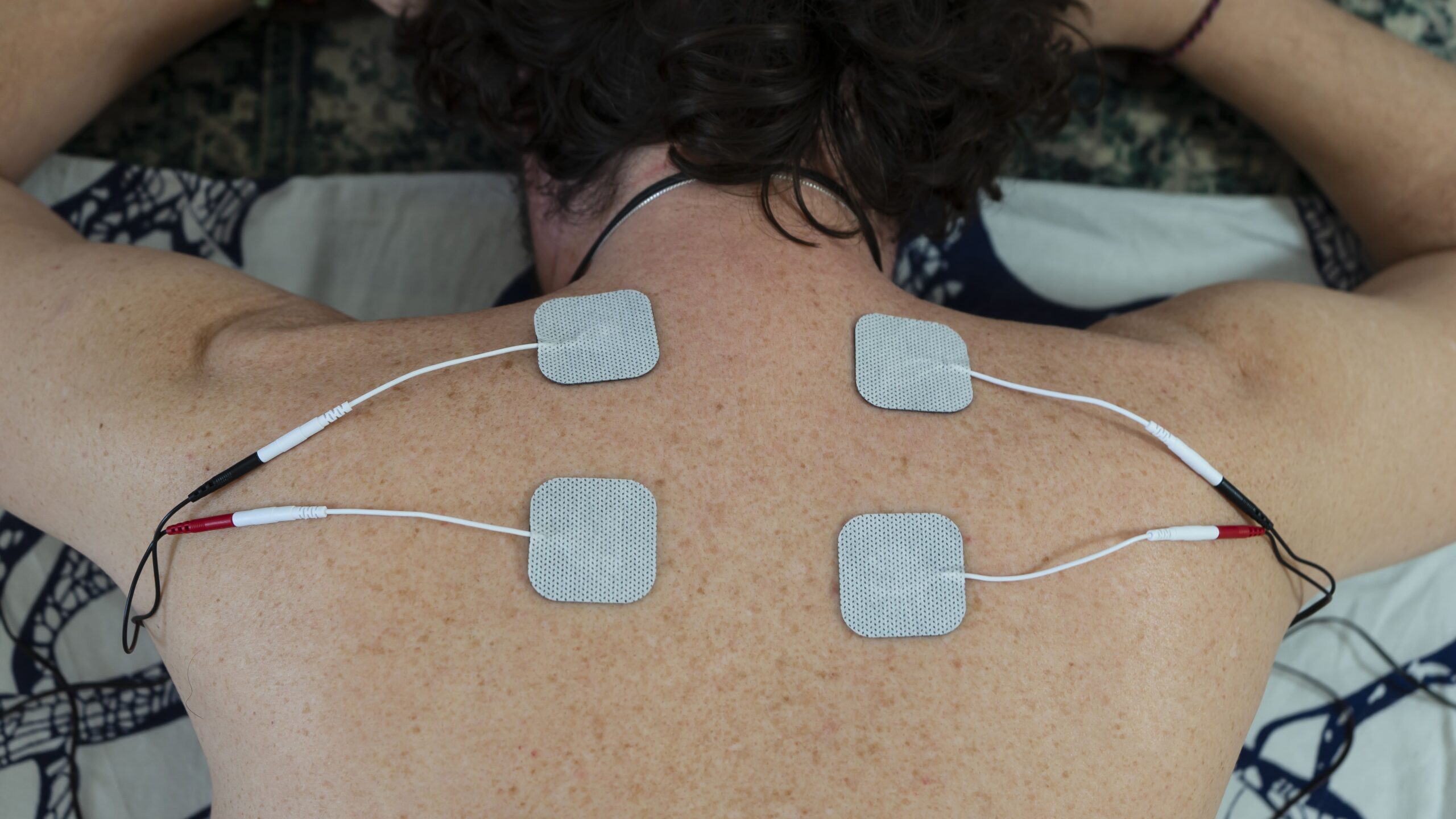
Microcurrent therapy is increasingly explored in rehabilitation and sports medicine for its potential role in recovery and workload management. Research examining delayed onset muscle soreness found that microcurrent-treated groups reported reduced soreness intensity and faster perceived recovery following intense exercise (Curtis et al., Journal of Athletic Training, 2010).
A review in Physical Therapy Reviews noted that microcurrent applications may support soft tissue recovery when integrated with physical therapy, although outcomes varied depending on protocol design and injury type (Johnson, Physical Therapy Reviews, 2016). This variability highlights the importance of individualized dosing, placement, and treatment cadence.
While the evidence base is still developing, interest continues to grow due to the low-risk profile and compatibility with existing rehabilitation frameworks.
Scar and Post-Surgical Tissue Support
Microcurrent therapy is sometimes applied during post-surgical recovery to support scar tissue remodelling and tissue quality. Small clinical trials and case series have reported improved tissue elasticity and reduced adhesion formation when microcurrents were introduced during later healing phases (Poltawski et al., Journal of Wound Care, 2012).
A separate observational report noted improved cosmetic outcomes and patient-reported comfort in post-operative patients receiving adjunctive microcurrent therapy (Becker, The Body Electric, 1985). However, high-quality randomized controlled trials remain limited, and current evidence supports its role as complementary rather than primary care.

Neuromuscular Applications
In neuromuscular rehabilitation contexts, microcurrent-based approaches are sometimes used to support muscle re-education without inducing forced contraction. Becker’s foundational work emphasized that nerve and muscle tissues respond to extremely small electrical signals, often far below sensory thresholds (Becker, The Body Electric, 1985).
Clinical applications focus on maintaining neuromuscular coordination and signalling efficiency in patients experiencing weakness, injury, or recovery-related inhibition. The objective is to assist natural signalling pathways rather than impose mechanical stimulation, distinguishing microcurrent therapy from traditional NMES approaches.

Clinical Workflow Considerations
Healthcare providers integrating microcurrent therapy typically follow structured clinical workflows to ensure safety and consistency.
Assessment involves confirming patient suitability and documenting baseline function. Contraindication screening excludes patients with pacemakers, active infections at the treatment site, or certain neurological conditions. Documentation includes tracking session parameters, patient response, and any adverse effects. Protocol planning tailors amplitude, polarity, waveform, frequency, and duration to the treatment goal.
Adhering to defined workflows supports reproducible outcomes and responsible clinical use across rehabilitation, wound care, and recovery settings.

Why This Matters
Microcurrent therapy is evidence-informed, safe, and increasingly versatile in healthcare. It complements, but does not replace, conventional medical treatments. Understanding applications, evidence, and workflow integration helps clinicians make informed decisions and sets realistic patient expectations.

